Call Today!
Coming Soon
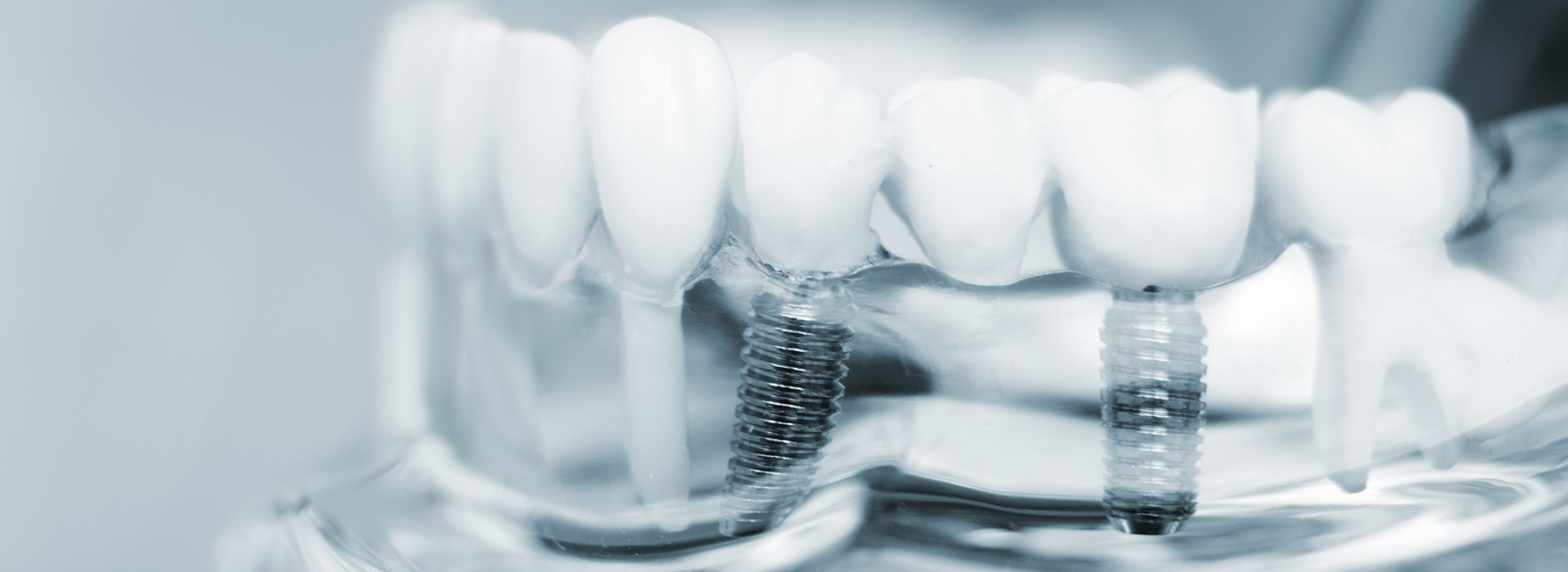
Missing teeth affect more than how you look — they change how you eat, how you speak, and how your jaw ages over time. Implant dentistry gives people a way to replace teeth with restorations that behave like real teeth: anchored in the jaw, stable under pressure, and designed to last. Whether a single tooth is gone or a full arch needs rebuilding, implant therapy is a predictable, well-established approach that restores both form and function.
At our Greenwood, IN office, the focus is on carefully planned treatment that balances long-term oral health with natural-looking results. The process starts with a thorough evaluation of your oral and general health, followed by tailored planning using digital imaging and precise diagnostic tools. This preparation helps ensure the implant is placed in the optimal position for both strength and aesthetics.
Implant restorations are particularly valuable because they replace the tooth root as well as the visible crown. That root-like support preserves bone, supports surrounding teeth, and maintains facial contours. This is why implant dentistry is often recommended when the goal is a solution that feels, functions, and looks like a natural tooth.
Unlike removable options, an implant is a small biocompatible post that integrates with the jawbone and becomes a stable foundation for a crown, bridge, or denture. This integration — called osseointegration — allows chewing forces to transfer through the implant into the bone, much like a natural tooth root. The result is improved bite function, better comfort, and a feeling of normalcy when eating and speaking.
Because implants sit below the gum line and interface with the jaw, they also support the surrounding bone. That stimulation helps prevent the bone loss that often follows tooth extraction, keeping the lower face fuller and preventing the gradual collapse that can occur with long-term tooth loss.
Modern dental implants are manufactured from medical-grade materials such as titanium or, in some cases, zirconia. Both materials are highly biocompatible and have decades of clinical success. Selection of implant material and design depends on factors like location in the mouth, bite forces, and any metal sensitivities — all of which are carefully considered during planning to prioritize predictable outcomes and patient safety.
Choosing implants is about more than aesthetics: it’s about restoring confidence, avoiding the complications of untreated tooth loss, and preserving long-term oral health. Implants eliminate many of the practical limitations of removable prostheses, such as slipping, food entrapment, and dietary restrictions, and they reduce the need to alter healthy adjacent teeth for support.
Because implant-supported crowns and bridges are self-supporting, they spare nearby teeth from being prepared or crowned simply to replace a neighbor. That conservative approach helps protect the health and structure of the remaining dentition while giving you a durable, functional result that integrates seamlessly with your smile.
For patients who have worn removable dentures, implants can be transformative. Anchored restorations reduce or remove the need for adhesives, improve chewing efficiency, and restore a sense of permanence that many people find liberating in daily life.
Implant dentistry is versatile: there’s a pathway for nearly every situation, from a single missing tooth to complex full-arch reconstruction. Treatment is individualized based on your oral health, bone anatomy, lifestyle, and goals. Below are the most commonly used approaches and how they are typically applied.
When only one tooth is missing, a single implant topped with a custom crown restores the tooth without affecting adjacent teeth. The crown is matched to your existing smile for a natural appearance, while the implant beneath provides root-like stability for normal chewing forces.
For multiple adjacent missing teeth, implants can support a bridge that spans the gap without relying on neighboring natural teeth for support. Strategically placed implants hold the fixed bridge in place and preserve bone while delivering a comfortable, long-term solution.
When an entire upper or lower arch needs replacement, implant-supported full-arch solutions offer fixed or removable options that outperform traditional dentures in stability and function. With careful planning, patients can receive temporary teeth quickly and transition to permanent restorations once healing is complete.
For denture wearers seeking improved retention, a few implants can be placed to anchor an overdenture. This hybrid approach provides significantly better stability than a fully removable denture while remaining serviceable and easier to clean for some patients.
A predictable outcome begins with thorough planning. That starts with a clinical exam, detailed imaging, and a discussion of health history and expectations. Digital X-rays or 3D scans help the clinician assess bone volume, locate vital structures, and determine the ideal position and size of each implant.
Surgery to place implants is typically performed in a comfortable outpatient setting. Many procedures are straightforward and completed under local anesthesia, with optional sedation available for patients who prefer it. Surgical time and complexity vary depending on the number of implants and whether preparatory procedures (like extractions or bone grafts) are needed first.
After placement, the implant integrates with the bone over a period of healing. During that time, a carefully managed recovery plan, pain control, and temporary restorations (when appropriate) help you maintain function and appearance. The final crowns, bridges, or dentures are fabricated with attention to fit, bite, and aesthetics once healing and integration are complete.
Clear communication is a central part of care. You should expect a detailed conversation about anesthesia and sedation options, step-by-step pre-op and post-op instructions, and a follow-up schedule that monitors healing and the health of surrounding tissues. This team-based approach reduces surprises and supports successful long-term results.
Long-term implant success depends on a strong foundation. When teeth are lost, bone in the area can shrink, and that loss may require grafting to rebuild adequate support. Bone grafting and related procedures are common and effective at restoring volume so implants can be placed in the right position for longevity and aesthetics.
Maintaining healthy gums and bone is equally important. Habitual factors such as smoking and uncontrolled systemic conditions can affect healing and integration, so candid conversations about lifestyle and medical history help shape realistic expectations and treatment sequencing. Periodontal health is evaluated and treated before implant placement when needed to reduce risks over time.
Once your implants are restored, caring for them mirrors the care of natural teeth: regular brushing, interdental cleaning, and routine dental checkups to monitor tissue health, occlusion, and the integrity of the restoration. Professional cleanings and periodic imaging help detect issues early so they can be addressed conservatively.
Implant restorations combine a durable foundation with tooth-colored materials designed for aesthetic harmony and wear resistance. With proper placement and ongoing care, implants are a long-term solution for many people. Regular maintenance visits and prompt attention to any changes in comfort or function are the best ways to protect your investment in oral health.

Implant dentistry offers a reliable path to restoring oral function and appearance while preserving the structures that support your face and bite. Whether you are exploring a single implant or considering a more comprehensive reconstruction, careful planning and skilled treatment give you the best chance for a durable, natural-looking outcome.
Our team at Unity Dental emphasizes individualized care, clear communication, and modern techniques to help patients understand their options and move forward with confidence. We aim to create treatment plans that reflect each person’s goals, health profile, and daily life so the result feels like the right fit for them.
If you’d like to learn more about how implant dentistry could restore your smile, please contact us for more information. We’re happy to answer questions and discuss the next steps toward rebuilding a healthy, comfortable bite.
If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are small biocompatible posts placed in the jaw that act like a tooth root to support a crown, bridge, or denture. Once the implant integrates with the bone through osseointegration, it transfers chewing forces into the jaw much like a natural tooth, improving bite stability and comfort. Because implants sit below the gum line, they also help support surrounding bone and soft tissues to preserve facial contours.
This root-like support distinguishes implants from removable prostheses by providing stability that reduces slipping and food trapping. Implants restore function for speaking and eating and can be designed to match the shape and color of adjacent teeth for a natural appearance. Long-term success depends on proper planning, placement, and ongoing oral hygiene to maintain tissue health around the implant.
Good candidates generally have adequate jawbone volume, healthy gums, and a commitment to oral hygiene and regular dental visits. Many systemic conditions can be managed in consultation with your dentist and physician, but uncontrolled medical issues or heavy tobacco use may affect healing and require tailored planning. A comprehensive exam including medical history, periodontal evaluation, and imaging helps determine candidacy and identifies any preparatory steps needed.
Age alone is not a limiting factor; suitability is based on oral and overall health rather than a specific number. Patients who wear removable dentures or who have lost one or more teeth often benefit from the improved function and stability implants provide. When additional procedures such as extractions or grafting are necessary, staged treatment can create the foundation needed for successful implant placement.
Careful planning begins with a clinical exam and detailed imaging, typically using digital X-rays or 3D cone-beam scans to assess bone volume, nerve position, and sinus anatomy. These diagnostics allow the team to select ideal implant size and position, often using virtual planning software to simulate outcomes and avoid critical structures. Health history and aesthetic goals are incorporated to create a customized treatment sequence that balances function and appearance.
When planning indicates additional procedures—such as bone grafting, extractions, or periodontal therapy—those steps are scheduled to optimize implant stability and long-term success. Clear pre-op instructions and discussion of anesthesia or sedation options are provided so patients know what to expect. This diagnostic groundwork reduces surprises and supports a predictable course from surgery through final restoration.
Most dental implants are made from medical-grade titanium, a material with a long history of successful use because of its strength and excellent biocompatibility. Zirconia implants are an alternative for patients seeking a metal-free option; both materials are chosen based on clinical needs, location in the mouth, and any patient sensitivities. Implant systems are subject to rigorous testing and clinical research to ensure predictable performance when placed and maintained appropriately.
Material choice is determined during treatment planning to support long-term stability and aesthetic outcomes. Your dentist will discuss the benefits and any trade-offs of different implant designs and restorative materials for crowns or bridges. Routine follow-up and proper oral hygiene are essential regardless of material to protect surrounding tissues and the restoration itself.
Implant surgery is usually performed in an outpatient setting using local anesthesia, and sedation is available for patients who prefer it to reduce anxiety. The procedure length varies with complexity but often involves placing one or multiple implants into prepared sites in the jaw, followed by suturing and a structured recovery plan. Initial healing typically takes a few weeks for soft tissue recovery, while osseointegration—the process of bone bonding to the implant—usually occurs over several months.
During healing, patients may receive temporary restorations to maintain appearance and basic function while protecting the surgical site. Pain is generally manageable with prescribed or over-the-counter medications and proper post-op care, and follow-up visits monitor tissue response and integration. Adhering to dietary guidance, oral hygiene instructions, and scheduled appointments helps support predictable healing and a successful final restoration.
Bone grafting is recommended when jawbone volume or density is insufficient to support an implant safely and predictably, which can occur after long-term tooth loss or following extractions. A graft rebuilds or augments the ridge so implants can be positioned for optimal function and aesthetics, and modern grafting techniques commonly use biocompatible materials to encourage new bone formation. For upper back teeth where the sinus cavity limits vertical bone height, a sinus lift can create the necessary space for implants by elevating the sinus membrane and placing graft material.
These preparatory procedures are routine and tailored to each patient’s anatomy and treatment timeline; some grafts can be performed at the time of extraction, while others are staged to allow healing before implant placement. The decision to graft depends on diagnostic imaging and the clinician’s assessment of long-term implant stability. With careful planning, grafting and sinus lifts significantly expand the number of patients who can benefit from implant-supported restorations.
Implant dentistry offers versatile restorative choices to address single missing teeth, several adjacent losses, or full-arch rehabilitation. A single implant with a custom ceramic crown replaces one tooth without altering neighboring teeth, while implant-supported bridges use strategically placed implants to support multiple replacement teeth when several adjacent teeth are missing. These fixed options provide superior stability compared with removable appliances and preserve surrounding tooth structure.
For patients missing an entire arch, implant-supported full-arch solutions can be fixed or removable and are designed to improve chewing efficiency and comfort compared with traditional dentures. Implant-retained overdentures use fewer implants to anchor a removable prosthesis, offering enhanced retention and easier hygiene for some patients. The selection of an approach depends on bone anatomy, aesthetic goals, functional needs, and the patient’s preferences discussed during planning.
Caring for dental implants mirrors the routine for natural teeth: brush twice daily with a soft brush, clean between teeth and implants daily with floss or interdental tools, and attend regular professional cleanings and examinations. Implant restorations and the surrounding tissues should be monitored for signs of inflammation, loosening, or changes in bite, and early detection of issues allows for conservative management. Good oral hygiene and consistent follow-up are the best ways to protect the health of the implant, bone, and gum tissue over time.
Patients should also maintain healthy habits that support healing and long-term success, such as smoking cessation and control of systemic conditions like diabetes. Your dental team will recommend a personalized maintenance schedule based on the type of restoration and your periodontal status. Promptly report any persistent discomfort, swelling, or difficulty chewing so the practice can evaluate and address potential concerns.
Like any surgical procedure, implant placement carries risks such as infection, localized bone loss, nerve irritation, or sinus complications depending on the site and anatomy. Most risks are minimized through careful diagnostic imaging, sterile technique, appropriate surgical planning, and thorough preoperative assessment of systemic health. When complications occur, early recognition and intervention—ranging from antibiotics and local care to revision procedures—help preserve implant function and surrounding tissues.
Long-term complications such as peri-implant mucositis or peri-implantitis can result from plaque accumulation or uncontrolled periodontal disease and require professional treatment to manage inflammation and protect bone. Regular maintenance, patient education on home care, and timely treatment of periodontal issues before implant placement reduce the chance of later problems. A collaborative approach between patient and clinician improves outcomes and supports implant longevity.
The practice emphasizes individualized care with detailed diagnostic planning, clear communication, and the use of modern imaging to guide predictable implant placement and restorations. Patients can expect a step-by-step review of their options, explanations of procedural steps, and tailored preoperative and postoperative instructions to promote comfort and successful healing. The team coordinates any necessary preparatory therapies—such as periodontal treatment or grafting—to create the best foundation for long-term implant success.
Dr. Sweety Patel and the clinical staff focus on minimally invasive techniques, patient education, and follow-up care to help patients make informed decisions and maintain their results. Appointments and ongoing maintenance are arranged through the Greenwood office to monitor integration, evaluate tissue health, and address any concerns that arise. This team-based approach is designed to deliver durable, natural-looking outcomes while prioritizing patient comfort and confidence throughout treatment.