Call Today!
Coming Soon
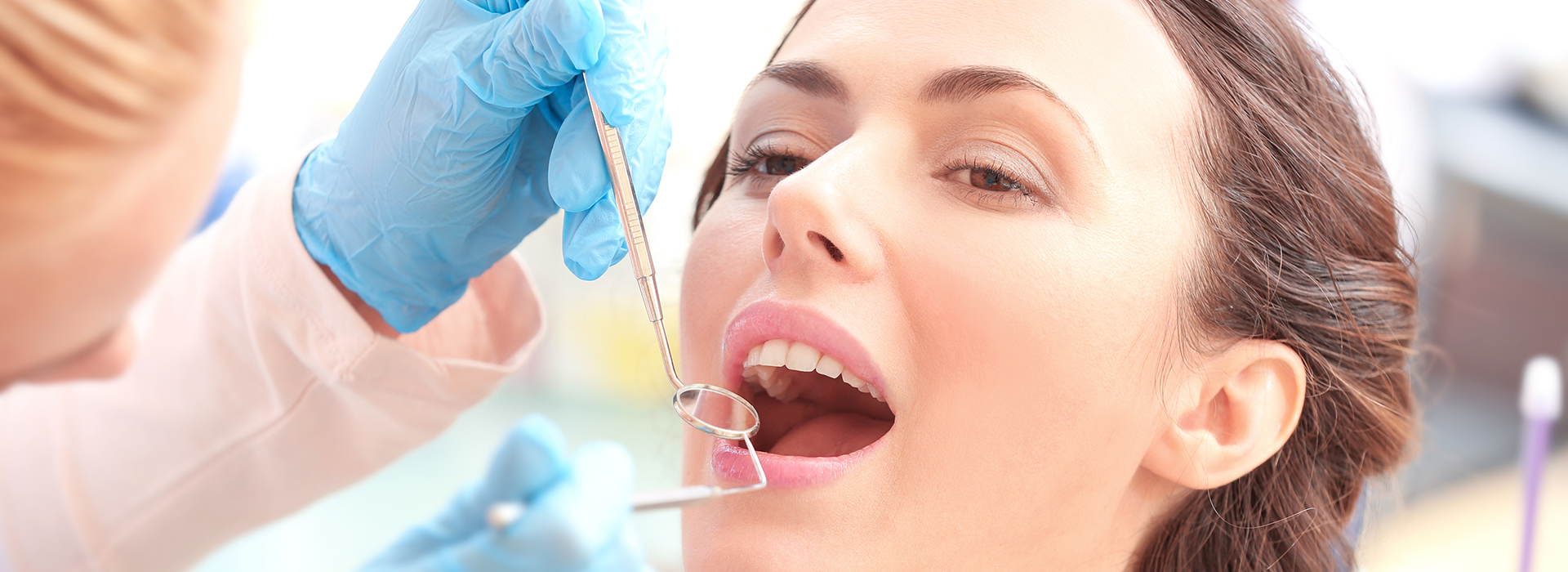
Gum disease is far more common than most people realize — and it’s the leading reason adults lose teeth. Research shows a large portion of adults experience some form of periodontal inflammation during their lifetime, yet early stages are often quiet and easy to miss. At the office of Unity Dental, our approach is to identify problems early, explain what’s happening in plain language, and work with patients to protect long-term oral health.
The periodontium is the name given to the gum tissue, periodontal ligament, and the underlying bone that anchor your teeth. When these structures are healthy, they keep teeth stable, protect nerve endings, and form a natural barrier against infection. When bacteria, plaque, and hardened deposits accumulate near and under the gumline, the resulting inflammation can erode these tissues over time.
Periodontal disease starts as a bacterial-driven inflammatory response. Left unchecked, that inflammation progresses quietly: collagen is lost, bone resorbs, and the spaces between tooth and gum deepen into pockets where bacteria thrive. Because early stages often cause little pain, routine exams and cleanings are the most reliable way to catch trouble before permanent damage occurs.
Awareness of how the periodontium functions helps patients appreciate why professional care matters. Simple daily habits reduce risk, but professional assessment and targeted interventions are the backbone of preventing progression and preserving teeth for the long term.
Gum disease develops when plaque — the sticky film of bacteria that forms on teeth — is not removed regularly. Over time plaque hardens into tartar (calculus) and the bacterial mix near the gum margins shifts toward more aggressive species. That change fuels inflammation, which in turn causes redness, swelling, and subtle changes in tissue attachment.
Because symptoms can be mild at first, we recommend paying attention to early warning signs so you can seek care before more invasive treatment is necessary. Common indications that a patient may have active periodontal problems include persistent gum bleeding, swelling, new tooth sensitivity, and a change in how teeth feel or fit together.
Common signs that warrant a professional evaluation include:
Gums that are red, puffy, or bleed with brushing and flossing
Chronic bad breath or an unpleasant taste in the mouth
Receding gum lines, exposed root surfaces, or teeth that feel loose
New spacing between teeth, changes in bite, or discomfort when chewing

Gum health connects to overall health in meaningful ways. Inflammation in the mouth can influence inflammatory pathways elsewhere in the body, and researchers have noted associations between periodontal disease and conditions such as cardiovascular disease, diabetes, and respiratory concerns. While the exact nature of these links continues to be studied, the consensus is clear: maintaining periodontal health supports broader wellbeing.
For patients with chronic medical conditions, controlling gum inflammation often improves comfort and can make systemic conditions easier to manage. Our team emphasizes coordinated care and clear communication with patients’ medical providers when appropriate, so oral health and general health goals align.
Prevention remains the most effective strategy. Regular professional cleanings, targeted education about home care, and timely treatment of early inflammation reduce the risk of tooth loss and help protect your overall health as you age.
Gingivitis is the earliest, reversible stage of gum disease. It is characterized primarily by inflammation of the gum margin without loss of bone or connective tissue. Patients with gingivitis typically notice bleeding during brushing or flossing, redness, or mild tenderness — but many people experience few or no symptoms, which is why exams matter.
If gingivitis is addressed promptly through improved oral hygiene and professional cleaning, the tissues usually return to a healthy state. This means that the body’s normal healing processes can restore the gum margin and stop the progression toward more destructive disease.
Our clinicians help patients develop practical, sustainable home-care routines and recommend evidence-based in-office therapies when extra cleaning is needed. Early intervention keeps treatment simple and preserves the natural support structures around teeth.

When gingivitis advances into periodontitis, inflammation leads to measurable loss of attachment and bone. Pockets deepen, and chronic infection can eventually allow teeth to loosen or shift. At this stage, preserving remaining tissue and stabilizing teeth become the primary goals of care.
Treatment shifts from purely preventive measures to organized therapy aimed at removing bacteria and creating an environment where healing and regeneration are possible. Depending on the extent of damage, this may include deeper cleaning beneath the gumline, localized antibiotic therapies, or surgical interventions to access and restore damaged areas.
Every treatment plan is individualized: our team assesses pocket depths, bone levels, and overall health to recommend a course of care that balances effectiveness with minimally invasive techniques whenever possible.
Modern periodontal care combines time-tested techniques with advances in technology to improve outcomes and patient comfort. Non-surgical approaches such as scaling and root planing remain foundational for removing subgingival plaque and smoothing root surfaces so inflamed tissue can reattach. When appropriate, adjunctive therapies — including locally delivered antimicrobials — support healing.
For cases where deeper pockets or bone loss are present, surgical and regenerative options can help restore anatomy and function. Procedures such as flap surgery, guided tissue regeneration, and bone grafting aim to reduce pocket depths, recontour tissues for easier self-care, and rebuild lost support where feasible.
Our clinicians also consider newer modalities like laser-assisted therapies in selected situations. These technologies can offer benefits for pocket reduction, peri-implantitis care, and precision tissue management, but the choice of tool always depends on clinical needs and predictable outcomes.
Successful periodontal care follows a sequence: accurate diagnosis, targeted treatment to remove bacterial burden and inflammation, and an individualized maintenance plan to prevent recurrence. Diagnosis includes a careful examination of pocket depths, bleeding on probing, tooth mobility, and radiographic assessment of bone levels. These findings guide the recommended therapy.
Periodontal treatment can be categorized in the following ways:
When disease is identified early, non-surgical therapies are often effective. Scaling and root planing remove plaque and tartar from beneath the gums and smooth the root surfaces so tissue can reattach. This approach minimizes tissue disruption while addressing the primary sources of inflammation.
Adjunctive measures — such as antiseptic rinses or locally delivered antibiotics — may be used to further reduce bacterial populations in difficult-to-reach areas. Close follow-up after these procedures helps determine whether healing is progressing or whether additional interventions are needed.
When pockets are too deep for non-surgical care, surgical techniques allow the clinician to access and thoroughly clean the root surfaces and reshape supporting tissues. Flap procedures provide visibility and access to remove stubborn deposits and, when indicated, facilitate regenerative steps to rebuild lost bone and connective tissue.
Reducing pocket depth and restoring supportive anatomy make daily hygiene more effective and reduce the chance of future breakdown. In select cases, dental lasers and minimally invasive surgical options can offer favorable healing with less postoperative discomfort.
At every step, we prioritize clear communication and realistic goals. Treatment is tailored to the patient’s oral and medical history, the extent of periodontal involvement, and personal priorities for preserving natural teeth and function.
In summary, periodontal care ranges from preventive cleanings that stop inflammation early to advanced procedures that rebuild and stabilize the tissues that support teeth. Early detection, consistent home care, and a collaborative plan between patient and provider are the best defenses against tooth loss and related health concerns. Contact us to learn more about how we can help you maintain healthy gums and a confident smile.
Most people don’t realize that periodontal disease is the leading cause of tooth loss among adults. According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease.
You may be surprised to learn that the human mouth is home to a wide variety of microbes. The fact is that over 700 different strains of bacteria have been detected in the oral cavity. Although some of these bacteria are beneficial, others are harmful to oral health. Without proper oral hygiene and routine dental care, these harmful bacteria can cause tooth decay and gum disease, compromising both your oral health and overall wellbeing.
In addition to inadequate oral hygiene and infrequent professional care, other factors, including smoking, genetic tendencies, and unchecked diabetes, can contribute to the escalation of periodontal disease.
Your gums and teeth have an interdependent relationship, which means healthy teeth depend on the support of healthy gums. Also, taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, respiratory problems, and adverse pregnancy outcomes such as pre-term and low birth-weight babies.
If you notice that your gums are bleeding with the slightest pressure while brushing or flossing, it’s a sign of gingivitis. Although gingivitis is the earliest stage of gum disease, it can easily be reversed with deeper cleanings as well as an improved regimen of oral hygiene at home.
In the absence of professional treatment and better home care, gingivitis progresses to the next stage, which is known as periodontitis. In this stage, the connective tissue and bone that hold the teeth in place begin to break down with an increase in pocketing between the teeth and bone, gum recession, and bone loss. Without proper treatment by your dentist, periodontitis will progress from a mild to moderate loss of supporting tissue to the destruction of the bone around the teeth.
Although gingivitis can often be reversed with improved oral hygiene and professional cleanings, as periodontal disease advances, more extensive procedures are required to halt its progression. Based on a complete assessment of your periodontal health and a review of possible contributing factors, our office will recommend the best options in care. Treatment for periodontitis may include a series of deeper cleanings known as root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser procedures, or antimicrobial medications.
The cost of care depends on the type of procedures required to restore your periodontal health. If you have dental insurance, plans often cover treatment to prevent gum disease as well as many procedures to treat the various stages of gum disease. Our goal is to help patients restore and maintain good oral health. We do all we can to help you begin care without additional stress or delay. Our business office works with you to maximize your benefits and provide easier, more convenient payment options.
By seeing our office regularly for care and doing your best to eat a healthy diet and practice good oral hygiene, you can keep your smile in tip-top shape as well as protect your overall wellbeing.
At the office of Unity Dental, we provide a comprehensive range of services to address all your oral healthcare needs. You can rest assured that your smile is in the best of hands at our office. Our skilled and experienced team maintains a position at the forefront of advances in care and remains dedicated to providing the highest quality of skilled and compassionate treatment.
Periodontal disease is an infection and inflammation of the tissues that support your teeth, including gum tissue, the periodontal ligament and underlying bone. It begins when dental plaque and tartar build up near and below the gumline and the bacterial balance shifts toward more aggressive species. That bacterial-driven inflammation damages collagen and bone over time, creating deeper pockets where bacteria can thrive.
Early stages such as gingivitis are reversible with proper care, but once attachment or bone is lost the condition is classified as periodontitis and requires professional intervention. Regular dental exams and cleanings are important because early disease often causes little pain but can progress silently. Understanding how the periodontium functions helps patients appreciate why prevention and timely treatment matter for long-term oral health.
Early signs of gum disease often include gums that bleed during brushing or flossing, redness, and mild swelling around the gum margins. Patients may also notice persistent bad breath, a metallic or unpleasant taste, or increased tooth sensitivity as the gums recede. These symptoms can be subtle, so they are commonly overlooked until disease progresses.
Other warning signs include new spacing between teeth, changes in how teeth fit together when you bite, and any sensation of looseness in a tooth. If you notice any of these changes, scheduling a professional evaluation helps determine whether treatment is needed. Early detection keeps treatment simpler and improves the chances of preserving natural teeth.
Diagnosis begins with a thorough clinical examination that includes measuring pocket depths, checking for bleeding on probing and assessing tooth mobility. Radiographic evaluation is used to assess bone levels and identify any areas of bone loss that are not visible during the clinical exam. Taken together, these findings allow clinicians to stage the disease and determine the appropriate course of care.
Medical history and lifestyle factors are also reviewed because systemic conditions and habits can influence periodontal health and healing. Based on the evaluation, the clinician will explain findings in clear language and recommend targeted treatments and follow-up. This diagnostic process ensures treatment decisions balance effectiveness with minimally invasive options when possible.
Non-surgical periodontal care typically starts with professional scaling and root planing to remove plaque and tartar beneath the gumline and to smooth root surfaces. This helps reduce bacterial burden and allows inflamed tissue to reattach, promoting healing of the periodontium. Adjunctive therapies such as antiseptic rinses or locally delivered antimicrobials may be recommended for hard-to-reach sites.
Follow-up evaluations after non-surgical therapy assess healing and determine whether further treatment is necessary. In many cases, improved home care combined with professional maintenance arrests disease progression and preserves supporting tissues. Close monitoring and individualized hygiene instruction are essential components of non-surgical management.
Surgical periodontal treatment is considered when pockets are too deep for effective non-surgical cleaning or when there is significant bone or connective tissue loss. Procedures such as flap surgery provide direct access to clean root surfaces and remove stubborn deposits, while regenerative techniques aim to rebuild lost bone and connective tissue where possible. Surgery may also recontour soft tissue to improve access for daily hygiene and reduce pocket depths.
Minimally invasive surgical options and technologies like lasers can sometimes reduce postoperative discomfort and speed recovery, but the choice of technique depends on clinical findings and predictable outcomes. Your clinician will discuss the goals, expected benefits and realistic limitations of any surgical approach. A clear plan for healing and maintenance follows surgical therapy to protect long-term results.
Research shows links between oral inflammation and systemic health, and uncontrolled periodontal disease may influence conditions such as diabetes and cardiovascular health. Although the exact mechanisms remain under study, reducing chronic oral inflammation supports overall wellbeing and can improve comfort for patients with certain medical conditions. Coordinated care and communication with medical providers are important when systemic health factors are present.
Managing gum disease can also reduce daily symptoms such as bad breath and sensitivity, which improves quality of life. Prevention and stabilization of periodontal disease are practical steps patients can take to support both oral and general health. Unity Dental emphasizes an integrated approach that considers patients' medical histories when planning periodontal care.
Recovery depends on the type and extent of treatment but commonly includes short-term tenderness, mild swelling and changes in bite sensitivity as tissues heal. After non-surgical care, many patients experience reduced bleeding and inflammation within days to weeks, while surgical procedures may require a longer healing period with specific postoperative instructions. Pain is typically managed with over-the-counter analgesics unless otherwise directed by the clinician.
Following postoperative guidance for oral hygiene, temporary dietary adjustments and any prescribed topical or local treatments supports predictable healing. Routine follow-up appointments let the team monitor tissue response and make timely adjustments to the care plan. Consistent home care and maintenance visits are essential to preserve treatment results over the long term.
Prevention centers on effective daily oral hygiene, including thorough twice-daily brushing and interdental cleaning with floss or other recommended devices. Professional cleanings at intervals determined by your clinician remove plaque and calculus in areas you cannot access on your own and allow early problems to be caught before they progress. Lifestyle measures such as tobacco avoidance and blood sugar control also lower the risk of disease.
Establishing a customized maintenance schedule is crucial after active therapy, because periodontal disease is chronic and prone to recurrence without regular care. Your clinician will set recall intervals based on disease severity, healing response and individual risk factors. Education and practical coaching help patients adopt sustainable routines that protect their periodontal health.
Contemporary periodontal care combines established techniques with adjunctive options to improve outcomes and patient comfort. Locally delivered antimicrobials, targeted antiseptics and host-modulation strategies can complement mechanical cleaning, while regenerative materials such as bone grafts and membranes support tissue rebuilding in appropriate cases. Laser-assisted therapies are also used selectively for pocket reduction and precision tissue management depending on clinical indications.
The choice to use any advanced modality is driven by the goal of predictable, evidence-based results rather than novelty alone. Clinicians evaluate the risks, benefits and scientific support for each adjunct before recommending it. Clear communication about why a particular tool or therapy is being used helps patients understand how it contributes to their care.
Personalized periodontal care begins with a comprehensive assessment that includes probing depths, radiographs, medical history and an evaluation of individual risk factors. Treatment recommendations are tailored to the extent of disease, patient goals for preserving natural teeth, and any relevant systemic health considerations. This individualized approach balances conservative methods with more advanced therapies when necessary.
Clinicians also prioritize clear explanations and shared decision-making so patients understand the proposed steps and expected outcomes. Ongoing communication and coordinated care with other health providers are used when systemic conditions influence oral health. You can expect a care plan that adapts over time as healing progresses and needs evolve at Unity Dental.